294/1 Asia Building (11th Floor), Phyathai, Bangkok
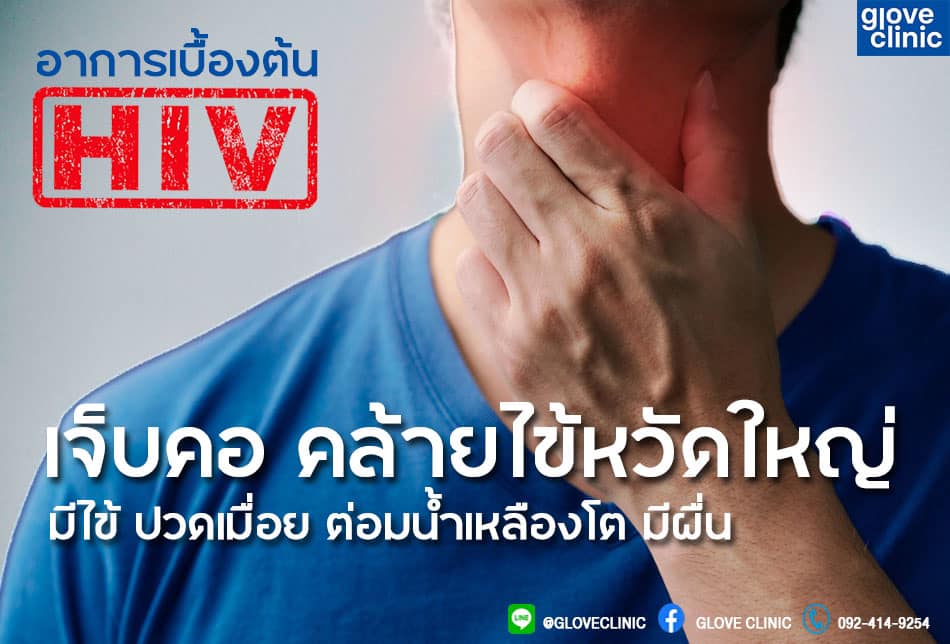
ตรวจ HIV รีวิวความรู้สำหรับการตรวจเอชไอวี (HIV test)
What is chlamydia?
Chlamydia is a common sexually transmitted disease (STD) caused by infection with Chlamydia trachomatis. It can cause cervicitis in women and urethritis and proctitis in both men and women. Chlamydial infections in women can lead to serious consequences including pelvic inflammatory disease (PID), tubal factor infertility, ectopic pregnancy, and chronic pelvic pain. Lymphogranuloma venereum (LGV), another type of STD caused by different serovars of the same bacterium, occurs commonly in the developing world, and has more recently emerged as a cause of outbreaks of proctitis among men who have sex with men (MSM) worldwide
How do people get chlamydia?
Chlamydia is transmitted through sexual contact with the penis, vagina, mouth, or anus of an infected partner. Ejaculation does not have to occur for chlamydia to be transmitted or acquired. Chlamydia can also be spread perinatally from an untreated mother to her baby during childbirth, resulting in ophthalmia neonatorum (conjunctivitis) or pneumonia in some exposed infants. People who have had chlamydia and have been treated may get infected again if they have sexual contact with a person infected with chlamydia.
What are the symptoms of chlamydia?
Chlamydia is known as a ‘silent’ infection because most infected people are asymptomatic and lack abnormal physical examination findings.
In women, the bacteria initially infect the cervix, where the infection may cause signs and symptoms of cervicitis (e.g., mucopurulent endocervical discharge, easily induced endocervical bleeding), and sometimes the urethra, which may result in signs and symptoms of urethritis (e.g., pyuria, dysuria, urinary frequency). Infection can spread from the cervix to the upper reproductive tract (i.e., uterus, fallopian tubes), causing pelvic inflammatory disease (PID), which may be asymptomatic (“subclinical PID”) or acute, with typical symptoms of abdominal and/or pelvic pain, along with signs of cervical motion tenderness, and uterine or adnexal tenderness on examination.
Men who are symptomatic typically have urethritis, with a mucoid or watery urethral discharge and dysuria. A minority of infected men develop epididymitis (with or without symptomatic urethritis), presenting with unilateral testicular pain, tenderness, and swelling.
Chlamydia can infect the rectum in men and women, either directly (through receptive anal sex), or possibly via spread from the cervix and vagina in a woman with cervical chlamydial infection. While these infections are often asymptomatic, they can cause symptoms of proctitis (e.g., rectal pain, discharge, and/or bleeding).
How is chlamydia diagnosed?
There are a number of diagnostic tests for chlamydia, including nucleic acid amplification tests (NAATs), cell culture, and others. NAATs are the most sensitive tests, and can be performed on easily obtainable specimens such as vaginal swabs (either clinician- or patient-collected) or urine. Vaginal swabs, either patient- or clinician-collected, are the optimal specimen to screen for genital chlamydia using NAATs in women; urine is the specimen of choice for men, and is an effective alternative specimen type for women.
What is the treatment for chlamydia?
Chlamydia can be easily cured with antibiotics. HIV-positive persons with chlamydia should receive the same treatment as those who are HIV-negative. Persons with chlamydia should abstain from sexual activity for 7 days after single dose antibiotics or until completion of a 7-day course of antibiotics, to prevent spreading the infection to partners. If a person’s symptoms continue for more than a few days after receiving treatment, he or she should return to a health care provider to be reevaluated.
Repeat infection with chlamydia is common. Women whose sex partners have not been appropriately treated are at high risk for re-infection. Having multiple chlamydial infections increases a woman’s risk of serious reproductive health complications, including pelvic inflammatory disease and ectopic pregnancy. Women and men with chlamydia should be retested about three months after treatment of an initial infection, regardless of whether they believe that their sex partners were successfully treated.
How can chlamydia be prevented?
Latex male condoms, when used consistently and correctly, can reduce the risk of getting or giving chlamydia. The surest way to avoid chlamydia is to abstain from vaginal, anal, and oral sex, or to be in a long-term mutually monogamous relationship with a partner who has been tested and is known to be uninfected.
Reference : https://www.cdc.gov/std/chlamydia/stdfact-chlamydia-detailed.htm
Make Appointment





Relate content :
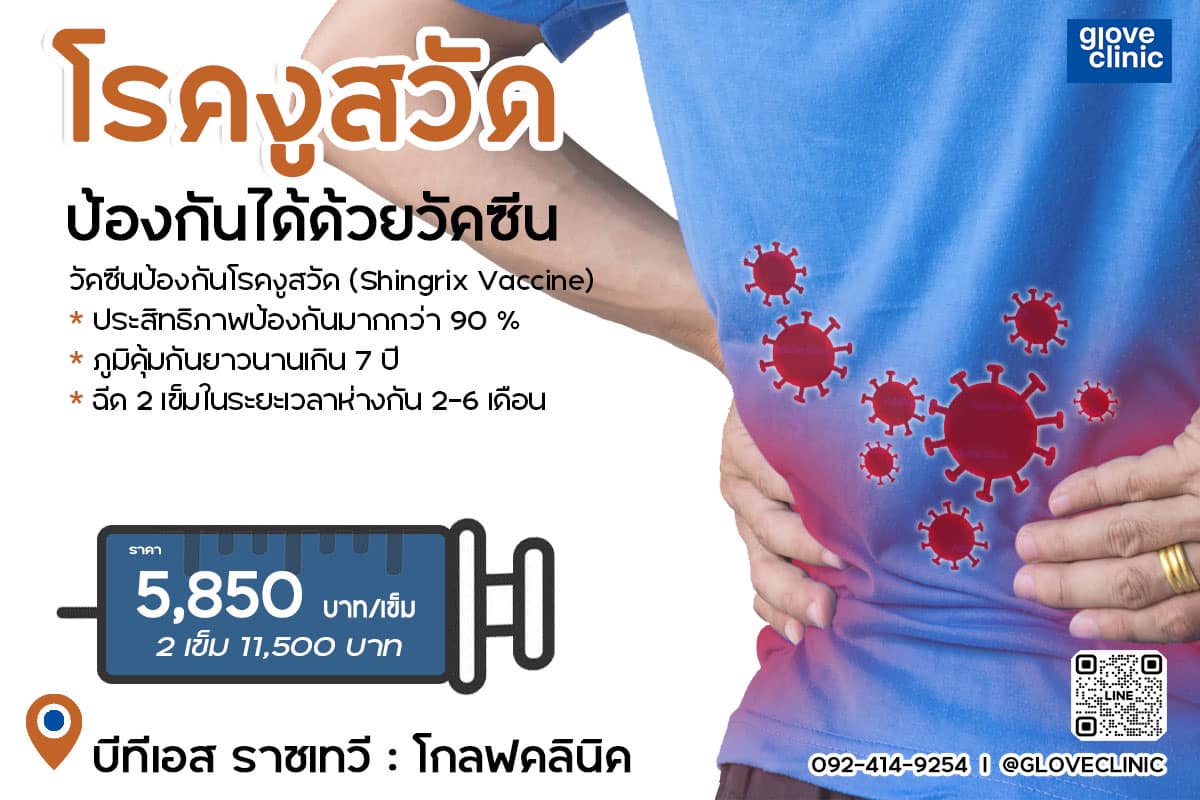
ฉีดวัคซีนงูสวัดที่ glove clinic
งูสวัดคือไวรัสชนิดหนึ่ง (Herpes zoster) ซึ่งเป็นเชื้อไวรัสตัวเดียวกันกับอีสุกอีใส (Varicella zoster) เมื่อเราติดเชื้อไวรัสอีสุกใสในวัยเด็กแล้ว ไวรัสสามารถที่จะหลบซ่อนได้ในร่างกายเป็นเวลานานหลายปี จนกระทั่งเมื่อร่างกายอ่อนแอ ไวรัสนั้นจึงออกมาทำให้เกิดอาการตุ่มน้ำใส ปวดแสบร้อนตามบริเวณที่เส้นประสาทต่าง ๆ ของร่างกายซึ่งเรียกกันว่างูสวัด
ตรวจ HIV รีวิวความรู้สำหรับการตรวจเอชไอวี (HIV test)
เอชไอวีคือไวรัสที่สามารถติดต่อได้จากการมีเพศสัมพันธ์, การใช้เข็มฉีดยาร่วมกัน, และการติดจากแม่สู่ลูก เมื่อติดเชื้อไวรัส HIV ไวรัสจะทำให้ภูมิคุ้มกันของร่างกายอ่อนแอลง และติดเชื้อโรคอื่น ๆ ได้ง่าย
ปีนี้มีคนไข้ป่วยด้วยไข้เลือดออกมากกว่า 2-3 ปีที่ผ่านมา
เนื่องจากว่าผู้คนกลับมาใช้ชีวิตปกติ มีการเดินทาง จึงพบการระบาดมากขึ้น โดยจากสถิติของกรมควบคุมโรคพบว่ามีผู้ป่วยด้วยไข้เลือดออกในประเทศไทยเกินกว่า 60,000 รายไปแล้วทั้งปี 2566 ไข้เลือดออกเป็นโรคที่ก่อให้เกิดความรุนแรงได้ทั้งในเด็กและผู้ใหญ่ โดยเฉพาะอย่างยิ่งในคนที่เป็นซ้ำครั้งที่ 2 จะมีโอกาสเกิดภาวะช๊อคและเสียชีวิตได้มากขึ้น (โอกาสเสียชีวิตอยู่ราว ๆ 1:1,000) วัคซีนไข้เลือดออกรุ่นใหม่สามารถครอบคลุมได้ทั้ง 4 สายพันธุ์และทั้งนี้ผลการศึกษาพบว่าช่วยป้องกันการติดเชื้อได้ถึง 80% และลดโอกาสการนอนโรงพยาบาลได้ถึง 90% นอกจากนี้ยังสามารถฉีดได้ทั้งในคนที่เคยและไม่เคยเป็นไข้เลือดออกมาก่อน (วัคซีนไข้เลือดออกรุ่นเก่าไม่ควรฉีดในคนที่ยังไม่เคยเป็นไข้เลือดออก) สอบถามข้อมูลเพิ่มเติมเรื่องวัคซีนไข้เลือดออกได้ที่ 092-414-9254, Line Official @gloveclinic (มีแอดข้างหน้า)
HIV แต่กำเนิด
ประเด็นร้อนที่ได้รับการพูดถึงอย่างมากในโลกออนไลน์ที่มีข้อความของนักศึกษาหญิงเปิดเผยว่าตัวเธอเองได้มีเพศสัมพันธ์แบบ one night stand เวลาไปเที่ยวกลางคืนบ่อยครั้ง และได้บอกความจริงว่าเธอเองมีเชื้อ HIV
อาการของเอดส์เป็นอย่างไร ทำความรู้จักกับเอดส์
เอดส์ คืออะไร แท้จริงแล้วเอดส์ไม่ใช่โรค หากแต่คือระยะสุดท้ายของการติดเชื้อ HIV ซึ่ง HIV นั่นเองคือไวรัสที่ทำลายภูมิคุ้มกันของร่างกาย โดยเซลล์หลักที่ถูกเล่นงานโดยไวรัสก็คือเม็ดเลือดขาว CD4 ซึ่งเป็นเซลล์ที่บัญชาการระบบภูมิคุ้มกันของร่างกาย ซึ่งเอดส์ในภาษาอังกฤษก็คือ AIDS ย่อมาจาก Acquired immunodeficiency syndrome กำเนิดของการเรียกชื่อว่าเอดส์ เดือนมิถุนายน ค.ศ. 1981 ในวารสารของกรมควบคุมโรค ประเทศสหรัฐอเมริกาได้รายงานว่ามีเกย์หนุ่ม 5 คนมีอาการปอดอักเสบจากเชื้อรา และได้รับการรักษาในโรงพยาบาลที่ Los Angeles โดย 2 รายเสียชีวิต และนอกจากนี้ทั้ง 5 คนยังพบการติดเชื้อไวรัส CMV และมีเชื้อราในช่องปากร่วมด้วย ซึ่งเชื้อต่าง ๆ ที่เล่ามานั้นมักเจอในผู้ป่วยที่มีภูมิคุ้มกันบกพร่อง ในขณะนั้นโลกยังไม่ได้รู้จักกับไวรัส HIV ว่าเป็นสาเหตุตั้งต้นของสิ่งที่เกิดขึ้น การเรียกภาวะนี้ในยุคแรกจึงได้เรียกว่า AIDS หรือ “เอดส์” ซึ่งย่อมาจาก acquired immunodeficiency syndrome อาการของเอดส์แตกต่างกับ HIV ยังไง เอดส์คือชื่อระยะที่ 3…